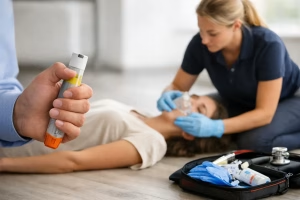
A severe allergic reaction rarely gives you much time to think. When someone’s airway is swelling, their breathing is worsening or they are showing signs of shock, staff need to recognise the problem early and act without hesitation. That is why an anaphylaxis response training guide should focus on practical recognition, clear decision-making and repeated hands-on practice, not just policy wording.
Contents
What good anaphylaxis response training needs to achieve
Anaphylaxis training is not simply about teaching what an EpiPen looks like. It needs to prepare people to spot a fast-moving medical emergency, call for help promptly and support the casualty while emergency services are on the way. In many workplaces, schools, leisure settings and community organisations, the challenge is not a lack of goodwill. It is uncertainty. People worry about getting it wrong, misreading symptoms or delaying because they are waiting for confirmation.
Good training reduces that hesitation. It gives learners a straightforward framework for responding to suspected anaphylaxis, while also making clear where local policy, job role and available equipment affect the response. A nursery, for example, may have individual care plans and known allergens on file. A construction site may be more concerned with remote access for ambulance crews and variable staff turnover. A sports club may need volunteers to manage both the casualty and the wider group at the same time.
Anaphylaxis response training guide for real-world settings
Any useful anaphylaxis response training guide should start with the fact that symptoms do not always present neatly. Some casualties show obvious airway swelling or severe breathing difficulty. Others begin with skin changes, abdominal symptoms, dizziness or a sudden sense of collapse. Staff need to understand that anaphylaxis can escalate quickly, and that a history of allergy matters, but should not be the only reason they act.
Training should cover the common signs of a severe allergic reaction in plain language. Difficulty breathing, wheezing, swelling of the tongue or throat, hoarse voice, persistent cough, pale or clammy skin, confusion and collapse all need urgent attention. In children, behaviour change can be an early sign, particularly if they become unusually quiet, distressed or floppy.
That said, training also needs some nuance. Not every allergic reaction is anaphylaxis, and not every rash means a casualty needs adrenaline. The aim is not to turn staff into diagnosticians. It is to help them recognise when the presentation is severe enough that they must treat it as an emergency, call 999 and follow their training without delay.
Recognition comes before equipment
A common weakness in first aid programmes is overemphasis on the device and underemphasis on assessment. Auto-injector practice is essential, but the first question is whether staff can identify that the casualty is deteriorating. If the early signs are missed, the best equipment in the room will not help quickly enough.
Scenario-based learning works well here. Learners should work through realistic examples relevant to their setting, such as a child after accidental food exposure, a staff member stung outdoors, or a gym user developing breathing difficulty after a known allergen contact. These examples help people connect symptoms, timing and escalation.
Staff must know exactly what to do next
Once anaphylaxis is suspected, the response pathway needs to be simple. Seek urgent medical help, assist with prescribed adrenaline auto-injector use if available and trained to do so, monitor airway and breathing, and prepare for further deterioration. If the casualty becomes unresponsive and is not breathing normally, basic life support becomes the priority.
This is where practical training matters. People need to rehearse how to call emergency services clearly, how to direct colleagues, how to retrieve medication, and how to monitor the casualty while waiting for the ambulance. In larger organisations, confusion often arises because everyone assumes someone else has made the call or fetched the device.
What to include in a workplace training plan
For employers, the right level of training depends on the risk profile of the environment. A low-risk office with no known allergy cases may not need the same depth as a childcare setting, hospitality venue or outdoor activity provider. Even so, relying on a single trained person is rarely enough. Absence, shift patterns and staff turnover can leave gaps very quickly.
A sound plan usually includes awareness for the wider team and more detailed practical training for nominated first aiders or those responsible for known at-risk individuals. Where there are personal care plans, staff should know where these are held and how they link to emergency action. Where there are shared spaces, such as canteens, clubhouses or training facilities, allergen awareness and reporting procedures also matter.
Training records should be current, easy to verify and tied to refresher dates. This is especially important in regulated or inspected environments, where employers may need to demonstrate both provision and competence. The certificate is part of the picture, but only part. Managers should also ask whether staff can still perform under pressure six or twelve months later.
Refresher intervals matter more than many teams expect
Anaphylaxis response is a skill that fades if it is not revisited. People forget device steps, lose confidence in symptom recognition or become unclear on whether workplace procedures have changed. A brief annual update can be more valuable than a longer session delivered once and then left untouched for years.
Short refreshers work best when they include hands-on trainer devices, a review of local emergency arrangements and one or two realistic scenarios. In settings with higher exposure risk, more frequent practice may be sensible. This is particularly true where volunteers, seasonal workers or part-time staff are involved.
Training methods that improve confidence
The most effective courses are practical, accredited where required and matched to the setting. Learners benefit from handling training devices, rehearsing verbal callouts and practising team roles. Written policies have their place, but they do not build the muscle memory needed in a high-stress incident.
There is also value in combining anaphylaxis content with broader first aid training. A responder who can recognise anaphylaxis but is unsure how to assess breathing, place a casualty appropriately or begin CPR is still only partially prepared. For many organisations, the safest approach is to integrate allergy emergency response into a wider first aid framework rather than treat it as a stand-alone topic.
This is where sector-specific delivery helps. A school needs examples involving children, care plans and parent communication. A marine setting may need to account for delayed access to ambulance crews. Forestry or outdoor teams may need to consider remote casualty management and site access. Training should reflect those realities rather than rely on generic classroom examples.
Common gaps that create avoidable risk
One of the most frequent issues is assuming that known allergies are the only concern. In practice, a first severe reaction can happen without a previous diagnosis. Staff should not ignore obvious signs of anaphylaxis simply because the casualty has no recorded history.
Another gap is poor medication access. If auto-injectors are locked away, stored inconsistently or known only to one member of staff, response time is lost. Training should include who holds medication, where it is kept and what to do if the first device does not resolve symptoms or a second device is available under the care plan.
Communication failures are also common. During an emergency, one person may stay with the casualty while another calls 999 and another clears access for responders. If nobody has rehearsed those roles, precious minutes can be wasted. Practical drills expose these weaknesses before a real incident does.
For organisations across Scotland, local delivery can make a real difference because trainers can tailor scenarios to the sector, the premises and the level of existing first aid provision. Providers such as SPR Training build this into delivery by focusing on accredited, hands-on instruction that reflects how teams actually work.
Choosing the right level of training
Not every team needs the same course, and that is where some employers either overbuy or underprepare. If your staff are responsible for children, vulnerable adults or clients with known allergies, a more structured and role-specific approach is usually justified. If your site already runs comprehensive first aid provision, anaphylaxis content may sit well within refresher or CPD training.
The key question is practical rather than theoretical. If a severe allergic reaction happened on your premises this afternoon, who would recognise it, who would act, and how quickly would the response start? If the answer is uncertain, your training plan needs work.
A useful standard to aim for is confidence with recognition, clear emergency action, familiarity with auto-injector use and the ability to support the casualty until ambulance crews take over. Beyond that, the exact training package should reflect your staff roles, risk profile and compliance requirements.
Anaphylaxis training is at its best when it removes doubt. People do not need dramatic language or overcomplicated protocols. They need credible instruction, realistic practice and procedures they can follow when the pressure is on. If your team can recognise the signs early and respond decisively, that training has done its job.
